To illustrate the measures we have put in place to keep our patients and staff safe throughout this pandemic, we are sharing the story of one of our patients, who came for shoulder surgery earlier this year. We detail their journey – through surgery, inpatient and outpatient physiotherapy – with the help of two of our physiotherapists
About Rochelle Francois
Rochelle Francois is a senior MSK and Upper limb Physiotherapist, who has a keen interest and experience in treating the shoulder, elbow and hand (upper limb). She has post-graduate certificates in Acupuncture, Pilates and is also a BAHT (level II) Hand Therapist who practices upper limb splinting. She enjoys treating a wide variety of post-operative shoulder & hand conditions.
About Daniel Bainton
Daniel completed his physiotherapy training in London and has extensive experience working in the NHS and private sector – this includes working internationally and at Premiership football clubs.
His specialist areas are shoulder and back pain, tendinopathies, post-surgical rehabilitation and strength and conditioning.
During the pandemic, tension has been extremely high. Our bodies are paying for the lack of true attention that we are giving to our overall health.
Some of us were able to focus on getting fitter during lockdown, eating better, spending time on relaxation and mindfulness. However, many of us are struggling with muscle, tendon and joint pain, but have been ignoring it as we are worried about going into hospital.
Due to the understandable concern over safety throughout this pandemic, on average the general population is attending far fewer hospital appointments than pre-pandemic.
This does not mean that fewer people are becoming unwell, that injuries are a thing of the past or that people are no longer suffering, but rather that these underlying issues are not being addressed or resolved as they could be.
With regards to musculoskeletal issues, delaying or avoiding seeing a healthcare professional could have an effect on your recovery, pain levels, ability to work, or on being able to carry out simple daily activities.
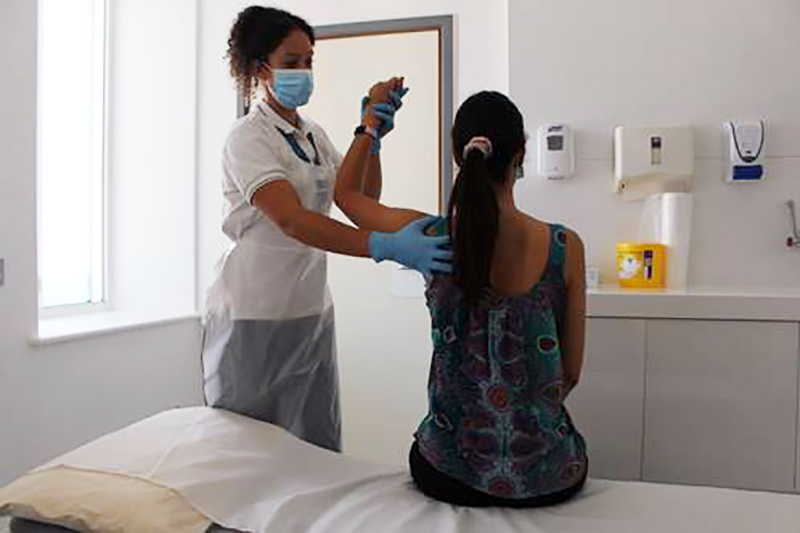
One of our recent patients was happy to answer questions about receiving physiotherapy treatment through the pandemic.
How did you come to have surgery during the pandemic?
The reason that I had surgery was because my surgeon told me that my condition would not resolve without it, and it would gradually get worse. The nerve was severely compressed and surgery was the only option.
I knew it was serious because of how weak my shoulder suddenly became. It literally felt like it happened overnight. I was unable to perform my duties at work or exercise in the same way that I was used to – I had never experienced anything like it before.
What support did you receive before your operation?
I wanted to ensure that I was as fit and strong as possible in the weeks before the surgery, because I knew this would give me the best chance of making a good recovery. I had a consultation with a Physiotherapist at The London Clinic and we agreed a programme of prehabilitation.
My ‘prehab’ involved a bespoke strength and conditioning programme – especially to optimise the strength of the remaining rotator cuff muscles that were working properly – alongside cardio and core exercises.
I was always pretty strong, but initially I couldn’t even do a plank or press-up because of the weakness and inhibition around my right shoulder.
However, by the time I had surgery, my strength was almost back to pre-injury level!
What happened before and on the day of your surgery?
I had to have a COVID-19 test and self-isolate for 14 days in order to have surgery in line with The London Clinic’s COVID-19 policy, which followed government guidance at the time.
Since then, the isolation period has decreased. I was getting used to it because of the pandemic, so was pretty well set up for self-isolating at home.
On the day of the surgery I attended hospital early and alone. It wasn’t an issue because I knew I was in good hands and would be going home later that day. I went down to theatres, I was put under general anaesthetic, and the next thing I knew I woke up with my arm in a sling.
How was your stay as an inpatient at The London Clinic?
During my stay I had a lovely nurse who looked after me really well. I also had a visit from the Physiotherapists, who readjusted my sling to make it more comfortable, reviewed my exercises and ensured that I was happy with everything before I went home.
I was a bit drowsy and my shoulder and arm were numb for most of the day, however it returned to normal in time for dinner.
How did you feel mentally and emotionally about having surgery during the pandemic?
I was due to have my surgery in spring but it was cancelled due to COVID-19. Finally, I was able to get it scheduled in June once government restrictions had lessened enough.
I understood why it had been cancelled and did not want to risk catching or spreading COVID-19 – however I was feeling frustrated and work was becoming challenging due to the lack of certainty.
Once the theatres opened in the hospital I was one of the first patients to be operated on.
Which measurements did you see in place at The London Clinic related to COVID-19?
When entering the hospital for the first time as an outpatient you are met at the door for a temperature check and given a face mask plus use of hand sanitiser.
You are only allowed to sit in chairs at least two metres apart in the waiting area in order to adhere to social distancing and there are strict, COVID-specific pathways that lead you up to the department that you require.
All staff wear face masks and extra PPE is worn by your healthcare professional.
How did you feel physically post-operatively?
Following surgery I regained movement really quickly. At two weeks, my surgeon told me that I had the movement of someone he would expect to see at six weeks post-op. This was reassuring and I have progressed every week since.
I had an online assessment with my Physio through The London Clinic’s secure platform called ‘Connect’, which worked really well. It meant that I didn’t need to make an unnecessary journey into hospital, and I started a graded return to work at six weeks post-op.
How did you feel coming in for face-to-face appointments?
The hospital is set up really well for outpatient appointments. Patients coming into Physiotherapy don’t have any contact with patients staying there. There are separate entrances and exits and the Physiotherapist comes to pick you up and take you back to the door.

Since I have been seeing my Physio for face-to-face sessions, my shoulder has continued to improve. The Physiotherapy gym is now open, which means we can use a variety of equipment. During my session today, my Physio assessed my shoulder and it is almost as strong as the other side.
I’m really pleased with how far I’ve come!
Further information
You can contact the Physiotherapy department directly on +44 020 7616 7651 or physio@thelondonclinic.co.uk if you would like more information on the services that we are providing at this time.





