The ongoing anxieties surrounding COVID-19 have resulted in many people feeling reluctant to visit their GP with minor complaints such as changes in bowel habits or skin moles. However, both can be early signs of something more sinister. This World Cancer Day, to raise awareness of both visible and invisible cancers, two of The London Clinic’s consultants highlight some key symptoms and what they mean for patient care
About Professor Siwan Thomas-Gibson
Professor Siwan Thomas-Gibson is a gastroenterologist and specialist endoscopist at St Mark’s National Bowel Hospital London. She is the Dean of St Mark’s Hospital Academic Institute and Professor of Practice in Gastrointestinal Endoscopy at Imperial College London.
About Dr Waseem Bakkour
Dr Waseem Bakkour is a Consultant Dermatologist specialising in Mohs micrographic surgery, skin cancer, lasers, general dermatology and cosmetic dermatology
Cancers of the upper and lower gastrointestinal tract (GI)
Professor Thomas-Gibson
The challenge with identifying upper and lower gastrointestinal (GI) tract cancers is that they are linked to symptoms that overlap with other less grave and more commonly known GI conditions such as irritable bowel syndrome (IBS).
Unfortunately, often the most tell-tale symptoms do not occur until the cancer progresses. It’s very important to discuss any of the following early warning signs of GI cancers with a healthcare professional as soon as possible to ensure they are investigated thoroughly, as often an early diagnosis will lead to much better outcomes:
- Unexplained abdominal pain
- Weight loss
- Fatigue (which may be due to anaemia)
- Blood in stools
- Change in bowel habit
Whilst many of us may know that the above red flag symptoms may mean something is wrong, it is worth knowing that 21% of bowel cancer patients see their doctor more than three times before they receive a referral – so if your issues continue, don’t be afraid to speak up.
This is also relevant for those under 50-year-olds who may not historically have been seen as ‘at risk’, but for whom bowel cancer incidence is now increasing.
Cancers of the upper GI tract, which includes the mouth, oesophagus (also known as the food pipe), stomach, and first part of the small intestine, are more of a challenge for healthcare professionals to diagnose.
There is no simple screening test, but symptoms can overlap those listed above with the addition of acid reflux or heartburn. This may indicate an issue in the food pipe.
When investigating for lower GI cancers, the first step your GP may ask you to take is to provide a sample of your stool for a faecal immunochemical tests (FIT).
To catch pre-cancerous lesions or cancers in their early stages, a healthcare professional may also view detailed images from inside the body via a procedure known as an endoscopy (colonoscopy or gastroscopy) or computerised tomography (CT) scan.
At The London Clinic we are fortunate to have a world class, JAG-accredited endoscopy suite and one of the largest independent specialist GI centres.
Our close team of experienced professionals includes some of the world’s leading endoscopists and radiologists, reassuring our patients that they will receive the very highest levels of care in our hands.
Detecting signs of skin cancer
Dr Wasseem Bakkour
Although skin cancer incidence has been on the rise consistently over the past decade, early detection is the key to a successful outcome.
It is therefore helpful for individuals to familiarise themselves with the ‘red flag’ signs of common skin cancers and speak with a healthcare professional if they have concerns.
Whilst the symptoms of common skin cancers can be easier to notice when compared with other types of cancer, rarer types of skin cancer can be challenging to pick up on. Here, I discuss some examples:
Basal cell carcinoma (BCC)
Basal cell carcinoma (BCC) often appears as a slowly growing pearly or red skin mark that commonly opens, scabs and bleeds. A rarer type known as morphoeic BCC can present like a white scar that feels hard and stiff to touch.
If your healthcare professional suspects BCC, you may be referred for a biopsy and removal of the growth.
Bowen’s disease
Bowen’s disease is an early pre-cancerous variant of squamous cell carcinoma – a common form of skin cancer – that is easily treatable since it usually appears as a red, scaly patch confined to the outer layer of skin known as the epidermis.
On the other hand, a full-blown squamous cell carcinoma usually presents as a rapidly growing red to skin colour lump. It usually has a central crust, can break open and bleed and is often painful. Both of these should be flagged to a healthcare professional urgently as a biopsy and removal may be required.
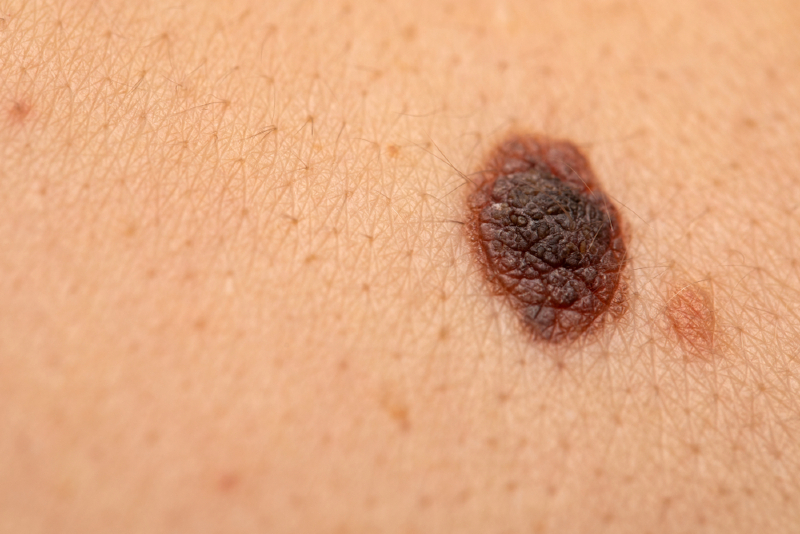
Melanomas
Melanomas arise on normal skin in the majority of cases (75%), usually as an irregular-shaped pigmented skin colouring with an irregular outline. The marking may include multiple shades of black, brown, blue and grey, and change relatively rapidly. They can then progress into a lump.
In about 25% of cases, melanomas appear as a change in a pre-existing mole with a history of change in size, shape and/or colour.
Rarely, melanomas can be pink in colour – this is known as amelanotic as it does not contain the skin pigment known as melanin.
Lastly, they can arise from the areas where our fingernails and toenails start to grow as a lengthwise streak across the nail.
In general, any new pigmented skin marks or a change in a pre-existing mole warrants a visit to a professional, who will be able to provide further advice and guidance on the next steps.
Further information
Digestive health services
Dermatology services





